This web page was produced as an assignment for an undergraduate course at Davidson College
Typhoid Fever
Typhoid fever is a systemic disease caused by an infection with Salmonella typhi, the typhoid gram negative bacillus which only infects humans. Typhoid fever affects 17 million people worldwide every year with approximately 600,000 deaths( Chin 2000). Typhoid fever in the developed world has been controlled by exemplary public measures such as sanitation and chlorination of drinking water. The developing world is plagued by problems such as poor sanitation, poverty, and war; therefore typhoid fever is able to causes 5% or more deaths in the developing world due to inhabitable condition (Pang et al. 1995). Typhoid fever is transmitted by food and water contaminated by the feces and urine of patients and carriers. Polluted water is the most common source of typhoid. In addition, shellfish taken from sewage contaminated beds, vegetables fertilized by night soil and eaten raw, and contaminated milk are another important sources of Salmonella typhi contraction. People with typhoid have bacterial replication in the reticulo-enodthelial system and significant inflammation of the lymphoid organs of the small intestine. Some symptoms of typhoid fever the sudden onset of sustained fever of the cases, severe headache, nausea, severe loss of appetite, constipation or sometimes diarrhea. Severe forms have been described with mental dullness and meningitis (Yano 2002). For example in research conducted in Hong Kong, China, fever was the most common symptom with 98.3% of the patients ( Chow et al. 1989).
Most current understanding of Salmonella typhi is from viewing the disease in humans, volunteer research and animal models. The murine model using Salmonella typhimurium is the best characterization of typhoid fever in humans (Passetti et al 2003). In murine's first exposure, the Salmonella typhi is ingested and it enters the small intestine via the microfold cells( M cells) of the Peyer's patches. After the M cells endocytose the Salmonella typhi, the bacteria able is able to migrate to the mesenteric lymph nodes and multiply( Janeway et al. 2002) . The bacteria is released into the blood stream so it can circulate systemically therefore giving the bacteria a chance to cause a systemic disease( Janeway et al. 2002). The Salmonella typhi is then taken up from the blood by antigen presenting cells such as the macrophages that line sinusoids of the liver, spleen, and bone marrow. In the macrophages, the Salmonella typhi is able to replicate and stay in the areas of the spleen, liver, and bone marrow( Diagle et al. 2001). The macrophages can loose the ability to kill the intracellular bacteria. Therefore T helper 1 cells with the Fas ligand can initiate the caspase pathway and kill the macrophage ( Janeway et al. 2002). The inflammation at the site of infection may be caused the production of Interleukin 1 , Interleukin 18 by caspase 1, TNF alpha, and the release of the contents of bacteria from the macrophages ( Brennan et al. 2000).When the bacteria is able to reenter circulation and make its way back into the blood, one is then able to view the clinical onset of the disease such as fever, nausea, constipation and diarrhea. The Salmonella typhi is then removed from the blood via the gall bladder to the small intestine.

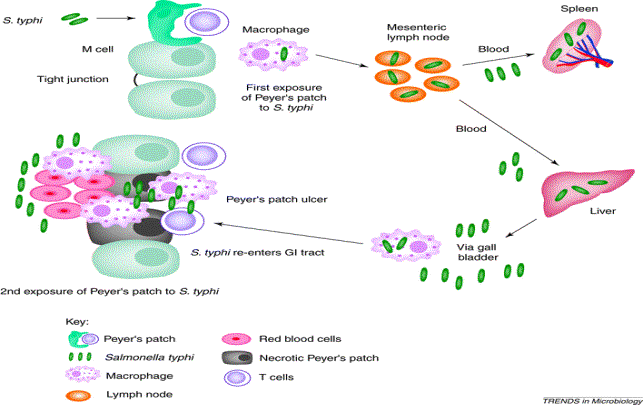
Figure 1.Salmonella typhi infecting the body via the Peyer's patches of the small intestine. The bacteria migrates to mesenteric lymph nodes and arrive via the blood in the liver and spleen during the first exposure. After multiple replication in the above locations, the bacteria Migrates back into the Peyer's patches of the small intestine for the secondary exposure and consequently the clinical symptoms are seen. Inflammation in the small intestine leads to ulcers and necrosis.( Permission received from P.Everest PhD on 04/24/03). P. Everest
As noted earlier, the Salmonella typhi is presented by macrophages. The macrophages present the molecules from the Salmonella typhi to CD4 T helper 1 but recent studies have also CD8 T cells involved in the response ( Salerone et al. 2003). When the bacteria reaches the Peyers patches a second time, The macrophages/ T helper and Cytotoxic CD8+ T cell accumulate and can try an kill the Salmonella typhi. The localization to the small intestine leads to Salmonella typhi being exposed a second time to Peyers patches causing inflammation, ulceration, and typhoid ulcers. The inflammation is once again caused by the release of cytokines such as Interferon gamma and tumor necrosis factor alpha , which lead to vascularization, the accumulation of more macrophages, and eventually necrosis ( Shtrichman et al. 2002). The ulcers can hemorrhage and this usually occurs during this time. The ulcerations are caused by the production of the enzyme, matrix metalloproteinases and this caused the loss of the mucuosal membranes in the small intestine (Macdonald et al. 2000). The loss of the mucosal membranes lead to ulcerations The Peyers patches perforate causing generalized peritonitis and septicaemia, the commonest cause of death .in typhoid fever (Butler et al. 1991).The death occurs in <5% of patients, but with a mortality approaching 40% and increasing substantially (83%) if treatment is delayed longer than 96 hours ( Van Basten et al. 1994).
People are often vaccinated with attenuated bacterial vaccine made of Salmonella typhi( Janeway et al. 2002).Some common treatments of typhoid fever are Chloramphenicol, Cotrimoxazole , and Quinolones (Kazemifar 2001). Chloramphenicol is an orally administered antibiotic first derived from cultures of the soil bacterium Streptomyces venezuelae. Cotrimoxazole on the other hand is an antibacterial agent that is a combination of two drugs that act together: Trimethoprim and Sulfamethoxazole to (Anderson et al. 1998). Lastly The quinolones are carboxylic acids and contain a quinolone ring that are used to treat infections of the intestinal tract( Anderson et al.1998). The primary treatments for Salmonella typhi can also be reused to treat a secondary reinfection of with the Salmonella typhi.
Anderson, P.O., and J.E.,Knoben .1998. Handbook of Clinical Drug Data. 8.
A.R.
Kazemifar. Treatment of Typhoid
Brennan, M.A., and
Cookson B.T. 2000. Salmonella induces macrophage death by caspase-1
dependent necrosis.
Molecular Microbiology., 38:31-40.
Butler, T., Islam, A., Kabir, L., and P.K., Jones. 1991.Patterns of morbidity and mortality in typhoid fever dependent on age and gender: review
of 552 hospitalized patients with diarrhea. Review of infectious disease.13:85-90.
Chin, J., 2000. "Control of communicable disease manual." American Public Health Association., 17.
Chow, C., Wang, P., and N.K. Leung.1989. " Typhoid fever in Hong Kong Children." Australian Journal of Pediatrics., 25(3): 147-150.
Diagle, F., Graham, J.E., and C.R., Curtiss. 2001. Identification of Salmonella typhi genes expressed within macrophages by selective capture of the transcribed sequences ( SCOTS). Molecular-Microbiology. 41(5):1211-1222.
Janeway, A.C, P. Travers, M. Walport., J.M. Shlomchik.2001. Immunology: The Immune System in Health and Disease. New York, NY: Elsevier Science Ltd. Garland Publishing, pp 387, 336, 586.
Macdonald T.T. , and L., Steidler. 2000 Recent developments in the immunology of inflammatory bowel disease. Journal of Immunology., 51:2-9.
Marcela F. Pasetti, Myron M. Levine and Marcelo B. Sztein. 2003. Attenuated Salmonella enterica serovar Typhi (S. Typhi) strains can serve as safe and effective oral vaccines to prevent typhoid fever Vaccine, 2003, 21:5-6:401-418
Pang T. and J.P. Johnson. 1995.
"Typhoid fever and other salmonellosis: a continuing challenge."
Trends Microbiology., 3:253-255.
Salerone, G.R., Wyant, T.L., Passeti, M.F., Fernadez, V.M., Tacket, C.O., Levin, M.M., and M.B., Sztein. 2003. Cocomitant induction of CD4+ and CD8+ T cell responses in volunteers immunized with Salmonella enterica serovar Typhi CVD 908-htrA.170(5):2734-2741.
Shtrichman, R., Heithhoff, D.M., Mahan, M.J., and C.E., Samuel. 2002. Tissue selectivty of interferon-stimulatied gene expression in mice infected with Dam + versus Dam- Salmonella enterica serovar Typhimurium strains. Infection and Immunity. 70(10):5579-5588.
Yano, Yuji.2002. "Typhoid fever and paratyphoid fever." Stomach and Intestine., 37(3).
Van Basten, J.P. and R. Stockenbrugger. 1994.Typhoid perforation. A review of the literature since 1960.Trop. Geogr. Med., 46:336-339.
Woodward TE, et J.K., Jung. Preliminary report
on the beneficial effect of Chloromycetin in the treatment of typhoid fever. Ann
Intern Med. 1948; 29: 131-134.