(Image taken from www.mayohealth.org)
Note: This
web page was produced as an assignment for an undergraduate course
at Davidson College.

(Image taken from www.mayohealth.org)
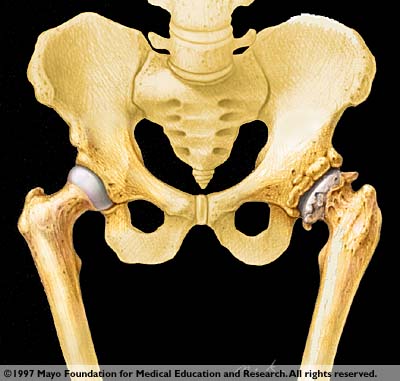
Figure 1. This image shows a normal
joint on the left vs. a joint affected by the deteriorating effects
of osteoarthritis. (http://www.mayohealth.org/mayo/9706/htm/osteoart.htm#ww5rn5).
Arthritis is an autoimmune disease. As defined by Charles Janeway, et al., an autoimmune disease is ìwhen a specific immune response is mounted against self antigens.î (Janeway 1999) How an autoimmune disease originates or what events lead up to this kind of response is unknown. There exist different types of arthritis: rheumatoid arthritis, septic arthritis, osteoarthritis,etc. In fact there exist over 100 different forms of this disease. The main characteristic of this disease is that it is either an inflammatory or degenerative disease that ultimately destroys the joints.
So, what is osteoarthritis? Osteoarthritis is the most common joint disorder; it is characterized by cartilage destruction and narrowing in the joint space. "As the cartilage breaks down, pieces may break off into the synovial fluid in the joint space. This will lead to further irritation and inflammation." (www.arthritisvic.org.au 2000) How this action begins is still unknown, however, the mechanism by which the cartilage is destroyed is known. Osteoarthritis mainly occurs in the hips and knees.
Articular cartilage absorbs stress and provides a smooth load bearing surface to permit low-friction movement of the joint. (Creamer 1997) The major structural protein of cartilage is type II collagen. Type II collagen maintains and binds the matrix molecules, IX and XI collagen, which are important for cartilage stability. (Creamer 1997) Another, and just as important, aspect of cartilage is the presence of aggrecan. Aggrecan, a macromolecule consisting of chondroitin and keratan-sulphate chains, is highly hydrophilic and of low viscosity--perfectly "suited for its function of load dispersal." (Creamer 1997)
Some believe that a predisposition to the disorder coupled with other factors like age, obesity, previous injury or surgery on the joint, excessive physical activities, and diet contribute to the onset of the disease. (Cooper 1999) However, relatively little is known of the roots of the pain and disability of osteoarthritis.
On a more molecular level, Nisha Manke and Nancy Lane in a recent issue of American Family Physician, penned it nicely when describing cartilage breakdown:
ìCytokines and growth factors are thought to play a role in the pathophysiology of the disorder. Interleukin-1 and tumor necrosis factor-beta may function to activate enzymes involved in the proteolytic digestion of cartilage. Growth factors such as tissue growth factor-beta and insulin growth factor-1 may play a role in the bodyís attempts to repair cartilage through cartilage synthesis. When catabolism exceeds cartilage synthesis, osteoarthritis develops.î (Manek 2000)
Synthesis of matrix metalloproteinases, collagen and proteoglycan degraders, are found in high concentration in cartilage effected by osteoarthritis. (Creamer 1997) Breakdown of cartilage is dependent on the stimulatory effects of interleukin-1 (IL-1). (Creamer 1997) Synthesis of cartilage is dependent on the growth factors, insulin-like growth factor-1 (IGF-1) and transforming growth factor b (TGFb). (Creamer 1997) High, normal and low concentration levels of IGF-1 have been found in human beings with osteoarthritis; so, it is not sure whether or not treatment of IGF-1 would be effective. (Creamer 1997)
The other characteristic of osteoarthritis, inflammation, is
not a clear subject either. It is possible that inflammation
is caused by expression of oncoproteins and nuclear factor-kB
(NF-kB), transcription factors for proinflammatory genes, in the
synovium; or caused by nitric oxide, found in cartilage chondrocytes,
a known inflammatory mediator released by IL-1. (Creamer
1997)
The predisposition to arthritis mentioned earlier is most likely
the result of genetics. Tim Spector of St. Thomasí
Hospital in London attributed the onset of osteoarthritis to environmental
risk factors but also noted that there exists a strong genetic
component to the disease. (Senior 2000) He attributed
this to studies involving twins. Spector noted a strong
correlation of osteoarthritis among monozygotic twins than among
dizygotic twins. (Senior 2000) John Loughlin, Institute
of Molecular Medicine in Oxford, England, suggested that an autosomal
dominant mutation in type II collagen could perhaps play a special
role in osteoarthritis. He also noted that genes linked
with osteoarthritis may not be limited only to cartilage.
His research has contributed to findings of susceptibility locus
for osteoarthritis on chromosome 11q, a region known to ìharbour
at least one gene that regulates bone mass.î (Senior 2000)
If the causes of osteoarthritis are relatively unknown, prevention becomes a bit difficult. Diagnosis of osteoarthritis occurs radiographically by measuring the narrowing of the joint. If one is diagnosed with osteoarthritis, the only idea that comes to mind is to control it, perhaps even stall the disease.
Physicians often recommend non-steroidal anti-inflammatory drugs (NS-AIDS) for relief. NS-AIDS come in two flavors: over-the-counter and available by prescription. Over-the-counter drugs include among others, Advil, Motrin, and aspirin. Prescription drugs include among others, Naprosyn, Relafen and Daypro. (Adderly 2000)
Other traditional methods of osteoarthritis treatment include regular calcium intake. Taking calcium several times a day is a common practice because it is believed, and has been proved, that that calcium deficiencies have been linked to osteoporosis.(Adderly 2000) Fractured bones, due to decreased levels of calcium, easily add to the discomfort of arthritis. By preventing osteoporosis, one is, in a sense, preventing potential harm to the bodyís joints. It has been recommended by Better Nutrition to eat more green foods.
As sited from an article dated January 2000, Gary Bushkin wrote:
ì1. Magnesium-rich chlorophyll in greens stimulates
the hormone calcitonin to boost calcium in bones by drawing it
from soft tissue.
2.Green foods provide ample vitamin K, which activates
osteocalcin, the key non-collagen protein in bones
needed to anchor calcium molecules.
3.Green foods contain sufficient boron required to activate
vitamin D, critical to calcium absorption.
4.Greeen foods are chock full of enzymes that easily release
calcium and other minerals.î (Bushkin 2000)
Greens are believed to be a better source of calcium than dairy foods because they do not contain the harmful steroids, hormones and antibiotics that can usually be found in such foods. (Bushkin 2000)
Another traditional method of osteoarthritis treatment is exercise. Although physical activity can sometimes be a potential cause of osteoarthritis, carefully chosen programs of exercise can be beneficial. The stronger muscles are, the more support the joint will have. Studies measuring the effect of an exercise program on pain levels, self-reported disabilities, observed disabilities resulted in small to moderate improvement of osteoarthritis in the knee and less improvement in the hip. (Miller 1999)
With the release of The Arthritis Cure, about three years, surged interest in the compounds glucosamine and chondroitin. (Tufts University Health and Nutrition Letter Jan2000) Glucosamine is believed to stimulate production of compounds called glycosaminoglycans and proteoglycans, the ìbuilding blocksî of cartilage. (Tufts University Health and Nutrition Letter Jan2000) Chondroitin is believed to aid in the decelerating of cartilage wear; chondroitin is a protein ìthat gives cartilage its ëspringyí quality.î (Tufts University Health and Nutrition Letter Jan2000)
Studies done at the University of Liege in Belgium revealed that compared with a placebo pill, patients who were administered glucosamine sulfate showed, after three years, stable joint space. The group that had taken the placebo pill showed a marked decrease in joint space. (Tufts University Health and Nutrition Letter Jan2000) These results do not confirm glucosamine as a miracle drug, although there is a correlation between glucosamine administration and halting of the degeneration of joint space. Dr. Ronenn Roubenoff, M.D. of the Tufts Universityís Human Nutrition Center on Aging expressed that with less pain, an individual will stand straighter and when an individual stands straighter, the joint space will look wider. (Tufts University Health and Nutrition Letter Jan2000) In other words, glucosamine may not be halting degeneration of the joint, but may in fact be decreasing pain.
As of now, however, the medical establishment ìas a whole ëwonít accept glucosamine or chondroitin till theyíre proven effective,î as noted by Hendersonville, North Carolina specialist Amal Das, M.D. (Tufts University Health and Nutrition Letter Jan2000)
An FDA approved drug, Rofecoxib, has been FDA approved for treatment of osteoarthritis and rheumatoid arthritis. (Manek 2000) Rofecoxib (Vioxx) is a selective COX-2 inhibitor. The enzyme cyclooxygenase (COX) is required for the synthesis of prostaglandins and thromboxanes. (Medical Letter1999) COX-1 is believed to be expressed in most tissues and is thought to protect the gastric mucosa. COX-2 is mainly involved in inflammatory response. (Medical Letter 1999) Rofecoxib is special in the sense that is targets only COX-2 and not COX-1, like past NS-AIDS. Gastric ulcers and affection of platelet function were noticed when COX-1 is inhibited. (Manek 2000) Six studies conducted with rofecoxib revealed a greater decrease in signs and symptoms of osteoarthritis when compared with placebo. (Medical Letter1999) Noted side effects of rofecoxib are nausea, diarrhea, dyspepsia and lower extremity edema. (Medical Letter 1999) Another side effect is rofecoxib's relief of menstrual pain. (Henderson 1999)
Among other treatments and remedies out there to help osteoarthritis
pain are:
-MSM (methylsulfonylmethane), an organic sulfur compound essential
for healthy skin, hair and muscles and reported to be an arthritis
pain reliever (Adderly 2000);
-Silicon supplements. Silicon (an element that makes up chondroitin)
deficiencies have been correlated with osteoporosis. (Adderly
2000)
-Magnesium supplements. Magnesium plays an important role
in calcium absorption and the body's ability to use calcium.
(Adderly 2000)
-Vitamin C. Vitamin C is important in cartilage production.
(Adderly 2000)
-Boswellia seratta resin. This resin found from trees in
India has been found to have anti-inflammatory properties rivaling
over-the-counter painkillers. (Adderly 2000)
-Capsaicin. A derivative of hot chili peppers, capsaicin
is rubbed on joints several times daily and shows decreasing joint
tenderness and pain. (Adderly 2000) Localized burning is
the only side effect. (Adderly 2000)
In short, osteoarthritis is a degenerative disease which will
never go away. Measures have been found to, at least, decelerate
progression but nothing has been found to completely halt progression
of the disease. The main attributes of osteoarthritis are
joint space reduction due to cartilage breakdown. It is
known how cartilage is broken down, however, and unfortunately
so, it is not known what prompts the breakdown. This is
perhaps the most saddening aspect of this disease, arthritis in
general, and other autoimmune diseases: the cause is unknown.
Patients living with the disease seek help, search the internet
and perhaps find the same information listed above. Some
drugs like COX-2 inhibitors, (rofecoxib and celecoxib, another
COX-2 inhibitor) are well known, FDA approved and are controlled.
However, other treatments, particularly alternative medicine have
found a niche in the anti-arthritis coalition. Introduction
of capsaicin, B. seratta resin and, to an extent, belief in the
function of non-FDA approved molecules like chondroitin and glucosamine
are sometimes just as important to patients as regulated and medical
establishment-approved drugs.
Adderly, Brenda. The promise of arthritis relief, naturally.
Better Nutrition. 62(3): 52-57, 2000.
Arthritis Victoria. What happens in arthritis? 2000. <http://www.arthritisvic.org.au/arthritis/osteoart.htm#what%20happens>.
Accessed 19 April 2000.
Bushkin, G. Uh-Oh. Osteo. Better Nutrition. 62(1): 24, 2000.
Cooper, C. and Coggon D. Physical activity and knee osteoarthritis.
Lancet. 353(9171): 2177-2179, 1999.
Creamer, P and Hochberg, MC. Osteoarthritis. Lancet.
350(9076): 503-510, 1997.
Geriatrics. Vitamin D levels linked to incidence of hip osteoarthritis.
54(9): 67, 1999.
Henderson. Osteoarthritis drug relieves menstrual pain.
Women's Health Weekly. 9-11, 1999.
Janeway CA, Travers P, Walport M, and Capra JD. Immunobiology:
The Immune System in Health and Disease. New York:
Garland Publishers, Fourth Edition, 1999.
Manek, N.J. and N.E. Lane. Osteoarthritis: Current concepts
in diagnosis and management. Amer Fam Physician. 61(6):
1795-1805, 2000.
Mauldin R.K. New Cox-2 inhibitor approved. Mod Medicine.
67(7): 56, 1999.
Medical Letter on drugs and therapeutics. Rofecoxib for
osteoarthritis and pain. 41(1056): 59-63, 1999.
Miller, K.E. Exercise can improve outcomes in osteoarthritis.
Amer Fam Physician. 60(9): 2659-2660, 1999.
Rose, V.L. Clinical briefs. Amer Fam Physician. 60(4): 1248-1252,
1999.
Senior, K. Osteoarthritis research: on the verge of a revolution?
Lancet. 355(9199): 208, 2000.
Tufts University Health and Nutrition Letter. A look at glucosamine
and chondroitin for easing arthritis pain. 17(11): 4-6,
2000.
Tufts University Health and Nutrition Letter. Can one substance
treat both osteoarthritis and depression? 17 (9): 3, 1999.
Return
to Davidson College Biology Homepage
Return
to Davidson Immunology Homepage
Return
to Al's Immunology Home Page
© Copyright 2000 Department of Biology, Davidson College,
Davidson, NC 28036
If you have any questions, please email me at alvichot@davidson.edu