
**This webpage was produced as an assignment for an undergraduate course at Davidson College**
Treatment and Future Directions
Treatment
According to Aoki et al. (2006), almost 90% of patients with HSV-2 have recurrent infections after their first outbreak. In addition, 38% of these patients experience six or more outbreaks per year (Aoki et al. 2006).
Cyclic and acyclic nucleoside analogues
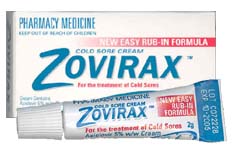
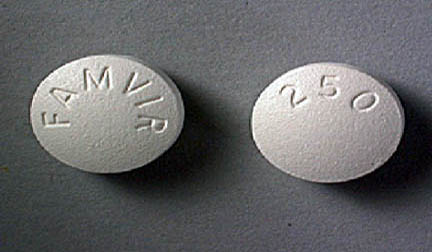
Nucleoside analogues target viral DNA polymerase. They are base pairs that are missing the 3’ hydroxyl group that is required to continue replication. These analogues compete with endogenous deoxyribonucleotides for insertion into the new DNA strand. When the analogue is inserted, viral DNA is stopped because the next nucleotide cannot be added. Examples of cyclic nucleoside analogues are Brivudin, which treats HSV-1, and Idoxuridine and Trifluridine, which treat HSV-1 and HSV-2. Acyclic nucleoside analgoues include acyclovir (Zovirax), famciclovir (Famvir), valacyclovir (Valtrex), and penciclovir, all of which treat HSV-1 and HSV-2 (see Figure 1). These medications are available in pill, topical, and IV forms. (Schang et al. 2006).
Patients with HSV have the option of going on antiviral continuously or intermittently (i.e. when they experience an outbreak). Those patients who experience frequent recurrences are often advised to take antivirals continuously, and using medication in this way reduces the risk of transmission. People who take these medications intermittently ingest pills twice daily for 2-5 days when they have outbreaks. However, a recent study found that patients who took famciclovir twice daily for only one day experienced faster healing by 2 days of genital lesions compared to patients who took a placebo. Patients who were able to start the medication within six hours of symptoms had the best outcomes (Aoki et al. 2006).



Figure 1. Images of HSV medications from:
www.sun-pharmacy.com/zovirax.shtml
opt.pacificu.edu/ce/catalog/14382-AS/Herpes.html
http://www.destinyrx.com/images/products/valtrex.jpg
Vaccine Development
Vaccines function through the creation of antibodies in the humoral immune response. However, antibodies against HSV are incapable of stopping infection and simply serve to minimize disease infection (Braun et al. 2006).
Vaccine development is focused on HSV-2 because most of the population already has HSV-1, and HSV-2 causes painful and unpleasant lesions in the genital region. However, there have been many problems in developing a vaccine against HSV-2 because of the latency period in the viral lifecycle. In addition, researchers still do not fully understand the mechanisms used by the immune system to prevent infection and reactivation (Aurelian 2004).
When vaccine research was first started, scientists hoped to create a vaccine that created both mucosal and global immunity since they believed that the creation of antibodies and T cells at the mucosa was the best way to stop HSV infection. Unfortunately, this strategy has not been successful, and vaccine research has instead been directed at minimizing the symptoms of primary HSV infection (Aurelian 2004).
According to Aurelian (2004), a vaccine that will work effectively against HSV-2 will induce Th1 immunity (as opposed to Th2), activate the innate immune response, and inhibit T regulatory cells. Th1 cells produce cytokines, such as IFN-γ, that suppress viral replication. In addition, vaccines can also be targeted against viral immediate early antigens because they are the first proteins produced in reactivation (Braun et al. 2006). Another protein target would be viral proteins that are produced during latency to prevent reactivation from ever occurring (Khanna et al. 2004).
Current vaccine candidates include protein subunits using glycoproteins as antigenic targets, killed virus, live recombinant virus, attenuated virus, and viral DNA vaccines. Human trials with the subunit vaccines resulted in the vaccine only being 70% effective in women who were seronegative for HSV-1 and HSV-2. Killed and attenuated virus vaccine studies did not have the correct controls (Aurelian 2004).
One vaccine approach has been against ICP10ΔPK. ICP10PK is a viral protein that upregulates Th2 cytokines and suppresses Th1 cells (Aurelian 2004). This protein is needed for viral replication and reactivation from latency, so researchers have targeted a vaccine against this protein. In clinical trials, ICP10ΔPK prevented HSV-2 recurrences in 37.5% of vaccinated patients and none in the non-vaccinated patients. In addition, the severity and frequency of recurrences was also reduced (Aurelian 2004).
A current vaccine undergoing clinical trials is termed the HERPEVAC trial. This vaccine targets viral gD and uses an adjuvant, which is deacylated monophophoryl lipid A from bacterial cell walls. Stanberry et al. saw that the efficacy of the vaccine was 73-74% in women who lacked antibodies for both HSV-1 and HSV-2. However, there was no protective effect in men. (Stanberry et al. 2002; Cunningham et al. 2006).
Figure 2. Vaccine. Image from http://www.doh.state.fl.us/disease_ctrl/epi/Epi_Updates/Epi_Weekly/01-07-05.htm
Future Directions
One major future area of research will be the vaccine development as described above. Overall, research that better identifies the way in which the cell-mediated immune system responds to HSV both in latency and initial infection will help to identify the most effective vaccine targets.
Davidson College Biology Department
Contact jehodge@davidson.edu with questions or comments.